
The Massachusetts Executive Office of Health and Human Services (EOHHS) recently selected Seven Hills Family Services (SHFS), an affiliate of Seven Hills Foundation, as one of nine Long Term Services and Supports (LTSS) Community Partners.
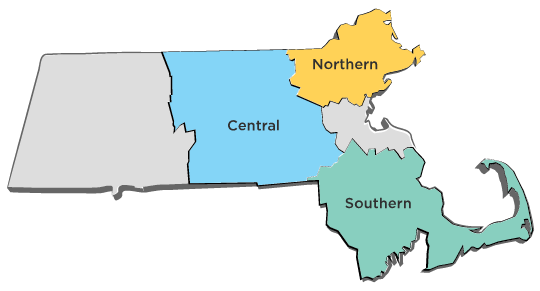 Doing business as Massachusetts Care Coordination Network (MCCN), Seven Hills is the lead agency collaborating with five LTSS partners, including Advocates, Brockton Area Multi Service (BAMSI), Horace Mann Educational Associates (HMEA), Boston Center for Independent Living (BCIL), and BayPath Elder Services (BayPath). MCCN will operate in the Southern, Central, and Northern Regions of Massachusetts.
Doing business as Massachusetts Care Coordination Network (MCCN), Seven Hills is the lead agency collaborating with five LTSS partners, including Advocates, Brockton Area Multi Service (BAMSI), Horace Mann Educational Associates (HMEA), Boston Center for Independent Living (BCIL), and BayPath Elder Services (BayPath). MCCN will operate in the Southern, Central, and Northern Regions of Massachusetts.
Throughout the United States, there are millions of Americans, including children, adults, and seniors, that are in need of long-term care services as a result of disabling conditions and chronic illnesses. Medicaid is the primary payer for these long-term care services. In fact, over 20% of Medicaid funding is directed to long term supports and services, including institutional care and community-based long-term services and supports.
Here in Massachusetts, this five-year community partners initiative is part of the Baker-Polito Administration’s response to the national Medicaid redesign through the Centers for Medicare Services (CMS) Innovation Funds. These community-based health care and human service organizations will partner with Accountable Care Organizations (ACOs) to integrate and improve member health outcomes of MassHealth (Massachusetts’ Medicaid program) members with complex long-term medical needs.
The Massachusetts Care Coordination Network is the largest LTSS Community Partner in the Commonwealth, and will utilize its extensive experience and expertise in providing care management and coordination to over 4,500 individuals in these three regions with long-term care needs to help them better manage their health and well-being, and improve their overall quality of life.
“We are excited to partner with EOHHS as well as our five affiliated partners and other subcontractors to implement this new care coordination system for individuals with long term support needs,” said Dr. Kathleen Jordan, Executive Vice President/Chief Executive Officer of Seven Hills Foundation. “Our work with the managed care entities statewide will result in a stronger system of care for all individuals and will work towards achieving the triple aim of healthcare reform efforts to improve care, improve health, and reduce costs.” LTSS Community Partners will receive funds from EOHHS for care coordination activities and to support infrastructure and capacity building. Significant investments will be made under the Community Partner model, including providing $145 million over five years to organizations providing care coordination support for people with complex long-term services and support needs. This includes members with physical disabilities, traumatic brain injury, intellectual or developmental disabilities, and others.
EOHHS’s specific goals for the LTSS CP Program include:
- Supporting Members with complex long-term care needs and their families to help them navigate the complex system of care in Massachusetts;
- Improving Member experience and quality of care for Members with long-term care needs;
- Creating opportunity for newly formed managed care entities (Accountable Care Organizations and Managed Care Organizations) to leverage the expertise and capabilities of existing community-based organizations;
- Investing in the continued development of long-term care services infrastructure;
- Improving collaboration across all partners to address social determinants of health such as housing, food insecurity, underemployment, and isolation, in order to deliver integrated care;
- Avoiding duplication of Care Coordination services for populations with long-term care needs;
- Supporting values of Person-Centeredness, Independent Living, aging in place, and cultural competence.
 Christine Lens, Director of MCCN
Christine Lens, Director of MCCN
We welome Christine Lens, RNc, MSN, MBA, as our Director for the Massachusetts Care Coordination Network (MCCN). Christine comes to MCCN with over 35 years of nursing experience; 25 years as a Nurse Practitioner. Christine’s experience encompasses new program development in community health centers to the delivery of high-quality patient care evidenced with improved quality outcome measures.



 Doing business as
Doing business as  Christine Lens, Director of MCCN
Christine Lens, Director of MCCN